Chronic rhinosinusitis with nasal polyps (CRSwNP) and allergic rhinitis (AR) are common upper-airway inflammatory disorders that often coexist, significantly decrease quality of life, and recur even when treated with intranasal or systemic therapy or surgery. Growing mechanistic insights, such as the role of type 2 inflammation driven by epithelial “alarmins” (TSLP, IL-25, IL-33) and downstream cytokines (IL-4/IL-13, IL-5), together with IgE-mediated effector pathways, have led to the accelerated clinical use of targeted biologics. Here, we summarize the shared immunopathogenesis of CRSwNP and AR, highlight treatable endotypes and practical biomarkers (e.g., blood eosinophils, total IgE, FeNO, and disease-specific symptom and quality-of-life scores), and map these features to therapeutic targets. We summarize evidence for approved agents, including anti-IgE omalizumab; anti-IL-5/IL-5R therapies mepolizumab, reslizumab, and benralizumab; and anti-IL-4R therapy dupilumab, focusing on clinically significant outcomes such as nasal polyp burden, nasal obstruction, olfaction, SNOT-22/TNSS improvement, reduction in systemic corticosteroid use, surgery rates, safety, and limitations. Given that many patients have multimorbidity with asthma or atopic dermatitis, we also outline how unified airway management can guide multidisciplinary decision-making and the use of shared endpoints. Practical considerations such as initiation criteria, response assessment, treatment switching, and economic or access barriers are summarized to inform real-world implementation and future research.

 1408 (Views)
1408 (Views)  461 (Downloads)
461 (Downloads) 
 1408 (Views)
1408 (Views)  461 (Downloads)
461 (Downloads) 
 436 (Views)
436 (Views)  156 (Downloads)
156 (Downloads) 
 418 (Views)
418 (Views)  248 (Downloads)
248 (Downloads) 
 365 (Views)
365 (Views)  231 (Downloads)
231 (Downloads) 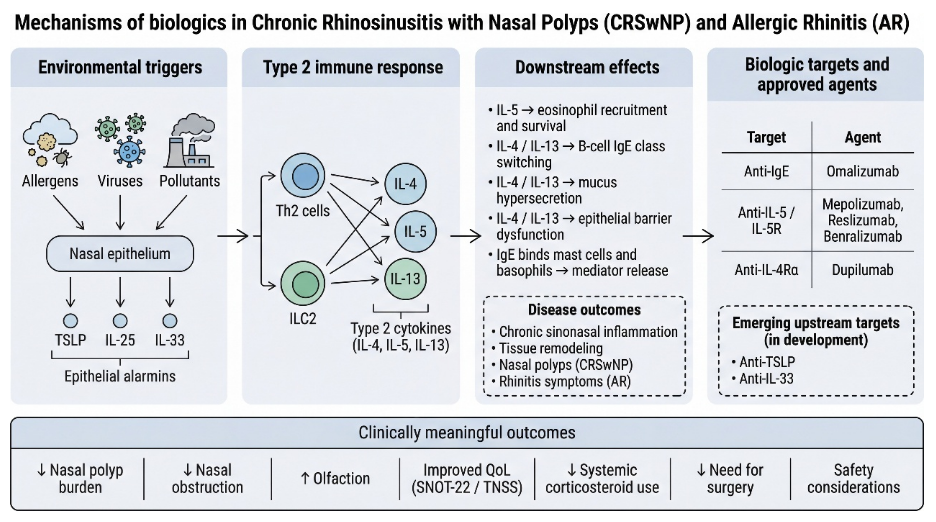
 427 (Views)
427 (Views)  229 (Downloads)
229 (Downloads)